Lecithin vs Choline for Recurring Plugged Ducts
Lecithin is out and choline is in. Previously, plugged ducts were thought to happen because milk simply “got stuck” in the ducts and needed to be massaged out. We now know the real culprit is localized inflammation, which narrows the duct and prevents milk from flowing, and therefore backs up behind the site of narrowing. This means our management strategies need to focus on reducing inflammation rather than just trying to push milk through.
So when new research shows that regular prophylactic lecithin supplementation can actually be inflammatory, it raises a critical question: why would we try to treat inflammation with something that we know is inflammatory?
Let’s dig in to when someone might still want to consider lecithin, and what safer alternatives exist for preventing plugged ducts.
The Theory Behind Lecithin
Despite how commonly lecithin is recommended for plugged ducts, there is no strong scientific evidence proving it is effective. However there are theories, like that of Jack Newman, that suggest lecithin may help prevent plugged ducts by decreasing the viscosity (stickiness) of breast milk. He proposes that lecithin may work by increasing the proportion of polyunsaturated fatty acids in milk, which could allow milk to flow more easily through the ducts. After all, it works as an emulsifier in the food industry, so why wouldn’t it do the same thing on our body.
One notable study found that adding soy lecithin to pumped human milk significantly reduced fat loss during enteral feeding as it prevented it from clinging to the edges of the feed tube. And although this research was not designed to study plugged ducts, it supports the idea that lecithin may be beneficial for fat dispersion within human milk.
What is Lecithin Anyway
Lecithin itself is not a single compound but a mixture of lipids, including:
choline
choline esters
fatty acids
glycerol
glycolipids
triglycerides
phosphoric acid
phospholipids such as phosphatidylcholine
It is the phosphatidylcholine, which plays a key role in maintaining membrane fluidity and emulsifying fats, helping fats mix evenly within liquids. Because of this property, lecithin is widely used as an emulsifier in the food industry and in infant formula manufacturing.
Typical Lecithin Dosage
Generally practitioners recommend taking 1200 mg, 3–4 times per day (3600–4800 mg total) when attempting to resolve a plug. Previously the recommendation was to then taper to a lower maintenance dose for prevention, but new recommendations suggest that if you are going to take lecithin that it should only be short term until the plug is resolved.
Why Should Lecithin Only Be Taken Short Term?
New research has found that when taken long-term (such as when used to prevent recurring plugged ducts) Lecithin is inflammatory. So when we know that plugged ducts are actually the result of ductal narrowing from the inflammation of surrounding tissue, why would we add in something inflammatory. Cue Choline, the active component of lecithin that helps fat dispersion within milk to reduce its viscosity and prevent fat aggregation.
Choline
Choline is the primary active component within lecithin. Lecithin supplements typically contain only about 1–2% choline, meaning very high doses are required to significantly increase intake of choline. Concentrated choline supplementation however (550 mg per day) removes the risk of worsening inflammation, and focuses on supporting fat transportation, cell membrane structure, and neurotransmitter production amongst other things. In the role of preventing plugged ducts, choline acts as a precursor for phosphatidylcholine, a major component of the milk fat globule membrane.
Recommended Choline Intake
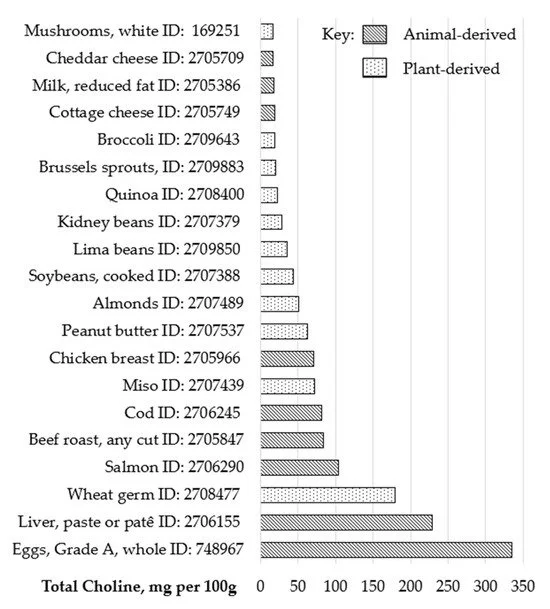
For all lactating individuals, the recommended daily intake of choline is approximately 550 mg per day, which can be obtained through diet or supplementation. Choline needs are critically high in both pregnancy and lactation, and most of us are not consuming enough of it. Knowing this, we make sure we are including foods rich choline such as eggs, salmon, beef liver, wheat germ, brussel sprouts, milk, shrimp, peanuts, and peanut butter.
Safety Considerations
Both lecithin and choline are generally considered safe (aside from lecithins inflammation that is), but caution is warranted in certain situations:
individuals taking blood thinners
people with soy allergies (sunflower lecithin may be preferred)
pregnancy, where high supplemental doses have not been well studied
individuals with gastrointestinal sensitivity
Some reports also suggest that very high doses of choline or lecithin may worsen mood symptoms in people predisposed to depression, so monitoring is recommended.
Before You Take Lecithin or Choline…
Before taking lecithin or choline, it is important to working with a skilled IBCLC to address potential causes or more serious cases including:
ineffective milk removal related to a poor latch or pumping issues
anatomical factors such as scar tissue, duct narrowing, or calcifications
infection such as mastitis or abscess that requires antibiotics
Evidence supporting lecithin for plugged ducts currently includes case reports, widespread clinical use, biochemical plausibility related to fat emulsification, and indirect evidence from neonatal nutrition studies. While this evidence is not definitive, it provides a reasonable theoretical basis for cautious clinical use when combined with comprehensive lactation care.
Sources
Chan, M. M., Nohara, M., Chan, B. R., Curtis, J., & Chan, G. M. (2003). Lecithin decreases human milk fat loss during enteral pumping. Journal of Pediatric Gastroenterology and Nutrition, 36(5), 613–615.
Irwin, C., Beard, K., Martin, L., Kua, K. L., & Huff, K. (2024). A simple step to improve fat and energy delivery of human milk delivered via bottle-feeding pump: An experimental study. Journal of Parenteral and Enteral Nutrition, 48(4), 686–692. https://doi.org/10.1002/jpen.2659
Sadovnikova, A., Greenman, S., Young, B., & Rosen-Carole, C. (2025). Recurrent nipple duct obstruction in two breastfeeding patients: A case report and discussion of the underlying pathophysiology. Journal of Mammary Gland Biology and Neoplasia, 30(2). https://doi.org/10.1007/s10911-025-09576-6
Wambach, K., & Spencer, B. (2021). Breastfeeding and Human Lactation (6th ed.). Jones & Bartlett Learning.
Zeisel, S. H., & da Costa, K. A. (2009). Choline: an essential nutrient for public health. Nutrition Reviews, 67(11), 615–623. doi: 10.1111/j.1753-4887.2009.00246.x; PMCID: PMC2782876.
National Institutes of Health, Office of Dietary Supplements. Choline Fact Sheet for Consumers. https://ods.od.nih.gov/factsheets/Choline-Consumer/
Naimi, S., Viennois, E., Gewirtz, A. T., et al. (2021). Direct impact of commonly used dietary emulsifiers on human gut microbiota. Microbiome, 9, 66. https://doi.org/10.1186/s40168-020-00996-6